
Community engagement matters for sustainable approaches to health challenges
Published on 15/09/2022

Simone D. McCourtie/World Bank CC BY 2.0
 This blog focuses on the ZOODLE word ‘PEOPLE’
This blog focuses on the ZOODLE word ‘PEOPLE’
When we talk about One Health, we often picture the classic Venn Diagram of human, animal and environmental health issues all overlapping one another. It’s this image that is displayed across our social media, publications, and researcher outputs to demonstrate how humans, animals and the environment are linked together in relation to health.
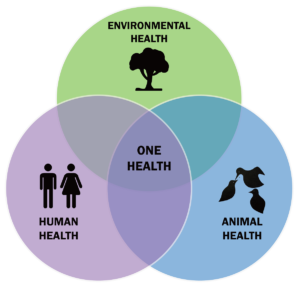
However, the terminology of humans can seem quite cold and removed from our lived experiences as communities, people, and individuals. It is these experiences which allow us to consider how One Health issues such as zoonoses, antimicrobial resistance (AMR), climate change etc. impact us and our surrounding environments and animals.
Lived experiences
As researchers it is therefore essential to engage with people at this very personal level to understand how lived experiences shape their impact on One Health issues. Community engagement (CE) interventions use different methods to allow people to share their knowledge and experiences around a certain problem and then co-create solutions or changes to behaviour.
People are families, communities, co-workers, animal owners, farmers, conservationists, travellers, professionals. It’s us as people that connect humans, animals, and the environment in both positive and negative ways. It’s people who must make difficult choices, for example degrading natural habitats to provide grazing space for their animals or deciding to use antibiotics as growth promotors to increase productivity and profit from their livestock. These choices often result in One Health challenges such as the spread of zoonotic infections from wild to domesticated animals or the spread of resistant bacteria up the food chain.
Without considering humans as people, it is difficult to empathise with and understand these actions, or to suggest meaningful solutions which protect the One Health space collectively from One Health challenges.
Community engagement

In the CE4AMR network we are particularly focused on the use of community engagement methodologies to understand the drivers of antimicrobial resistance in low- and middle-income country (LMIC) communities. We use methods such as participatory video and community dialogues to connect with people to better understand what choices are being made around antimicrobial purchasing and usage, and how these behaviours could be modified to minimise AMR risks.
This often means we may not be promoting a fully optimal behaviour in academic terms, because that behaviour is not contextually possible to the people we are working with. For example, suggesting people in rural communities only buy antimicrobials with a prescription can be very difficult to put into practice if these people do not have access to health professionals who issue prescriptions. In this case we may focus on empowering community people to ask specific questions about their illness and treatments so that they fully understand the medicines they are taking, how long to take them for and what to do if they don’t feel better.
Equally, in relation to zoonoses it is important to understand the reasons why people may be consuming bush meat or keeping animals in housing which is not secure from wildlife. There are often many more complex reasons than simply not knowing that this is a problem.
Humans can learn new behaviours and to tackle One Health challenges, but it is the people that need to put these into practice and this practice will be influenced by context. If it is a choice of imperfectly housing your livestock to keep them safe from predators despite bats roosting above them, or letting the animals roam free with little physical security, people are likely to take the first option as it provides them with immediate income and food security.
However, this is not to say that adjustments cannot be made, once we understand why a behaviour is happening and what drives it. We have seen successes in the way humans have been engaged on the issue of the climate crisis because we have worked with them as people; understanding what is meaningful in context and relating this back to how people, animals and nature are interconnected in certain settings. This has allowed communities and people to make environmentally sound choices based on their own experiences and knowledge.
Sustainable approaches
We now need to transfer this learning to other key One Health issues, AMR and zoonoses being two of the most pressing concerns. For a wider discussion of the application of climate crisis approaches to other global challenges take a listen to this podcast.
In summary, person-centred and community engagement approaches to One Health challenges are essential if we wish to develop meaningful and sustainable solutions to issues like AMR and zoonoses. Humans are people and we are connected to our environments and animal life in many ways based on context and situation. It is important for research teams to fully explore this issue of context when attempting to tackle a One Health challenge. This offers a route to developing bespoke solutions which can be delivered by the people experiencing said challenge, ultimately offering more sustainable action.





