
Introducing a bacteria that is both friend and foe
Published on 22/09/2022

TANUVAS
 This blog focuses on the ZOODLE word ‘ECOLI’.
This blog focuses on the ZOODLE word ‘ECOLI’.
The bacteria Escherichia coli (E. coli) is a member of the family known as Enterobacteriaceae (‘gut bacteria’) and is commonly found in the lower intestine of warm-blooded animals. Here, it usually lives harmlessly as part of a healthy microbiome, helping to produce vitamin K and actually protecting against colonisation by pathogenic (disease-causing) bacteria.
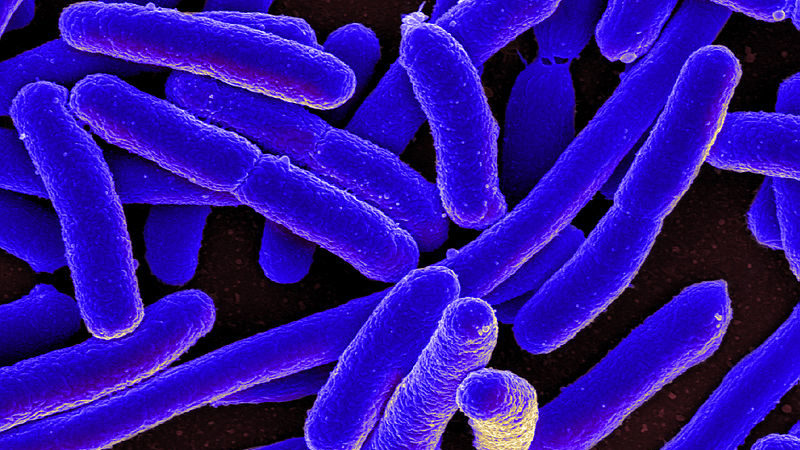
However, in the wrong place in the body, virulent strains of E. coli can be the cause of disease themselves in both people and animals. Different sub-types result variously in severe abdominal cramps, diarrhoea, hemorrhagic colitis, vomiting and/or fever. In rare cases, it can cause very severe disease, even death.
The most common route for E. coli infection is the faecal-oral route, when it can lead to food poisoning. Poor hygiene and cross-contamination are the major causes of such E. coli contamination. For this reason, E. coli is considered an indicator organism to test environmental samples for faecal contamination.
Poultry, as warm-blooded animals, carry E. coli naturally in their gut. Usually this does not cause a problem but the bacteria can cause the disease known as colibacillosis when birds are stressed, such as when overcrowded, malnourished, immunosuppressed or subject to poor ventilation or extreme temperature . Colibacillosis is one of the main causes of economic losses in the poultry industry.
Antimicrobial resistance
E. coli strains are also potential reservoirs of antimicrobial resistance (AMR) genes and so are considered to be excellent indicators to monitor the general level of AMR in bacterial populations. Research shows a high level of E. coli-originated resistance to antimicrobials in animals, including products considered critically important for people such as ciprofloxacin and colistin. Overuse and misuse of antimicrobials in animals and people increases risk for the selection of AMR in the naturally occurring E. coli found in the lower gut.
As a result of horizontal transfer of AMR genes, AMR in these E. coli may serve as an early warning for the development of resistance in disease-causing bacteria. AMR E. coli can transfer from food animals to people through direct contact or indirectly through the food chain.
One indicator is Extended Spectrum Beta Lactamase (ESBL) producing E. coli (ESBL EC). The World Health Organization (WHO) choose ESBL EC for its integrated global surveillance on AMR across the human, animal and environmental sectors as a relevant and representative proxy for the magnitude and trends of the global AMR problem.
Furthermore, the widespread use of newer antimicrobials such as carbapenem and colistin has been increasing in recent years, promoting selection of resistant E. coli for which none of the current antimicrobials are effective. Therefore, antimicrobials should be used prudently, not only in humans but also in animals and the environment.
In the One Health Poultry Hub we are isolating E. coli from chickens reared in different production systems in Vietnam, India and Bangladesh, as well as the human populations that surround them. Sequencing the genomes of these E. coli and the microbial populations they have been isolated from allows us to explore the occurrence of AMR genes and the risk of their flow through food chains to human populations.
Understanding the occurrence and flow of AMR genes can help us to safeguard the health of people as well as animal health and welfare.


